Revenue Cycle Management Market Analysis & Forecast: 2026-2033
Revenue Cycle Management Market is estimated to be valued at USD 196.91 Bn in 2026 and is expected to reach USD 440.78 Bn in 2033, exhibiting a compound annual growth rate (CAGR) of 12.2% from 2026 to 2033.
To learn more about this report, Request Free Sample
Key Takeaways
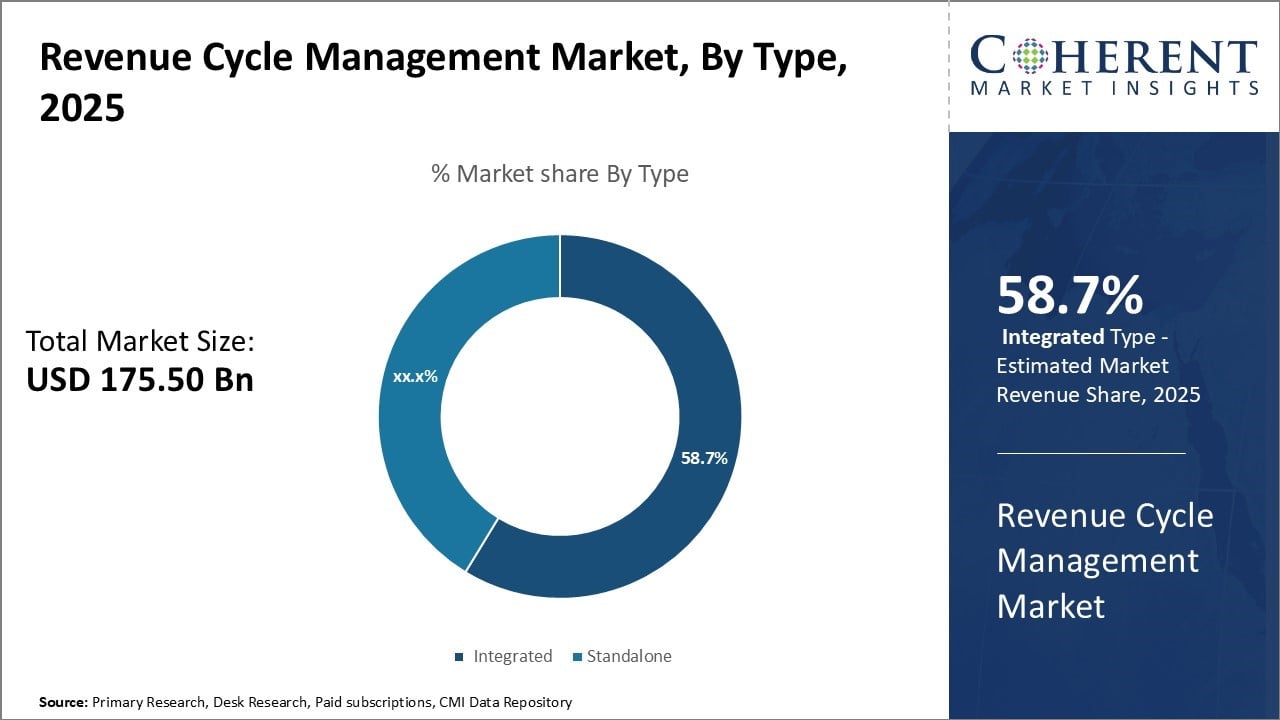
- According to Type, The Integrated Category is anticipated to account for the largest share of 59.7% for the Revenue Cycle Management market in 2026. Clinical and administrative procedures are unified by integrated revenue cycle management (RCM) systems, which simplify patient collections, billing, coding, and claims administration on a single platform.
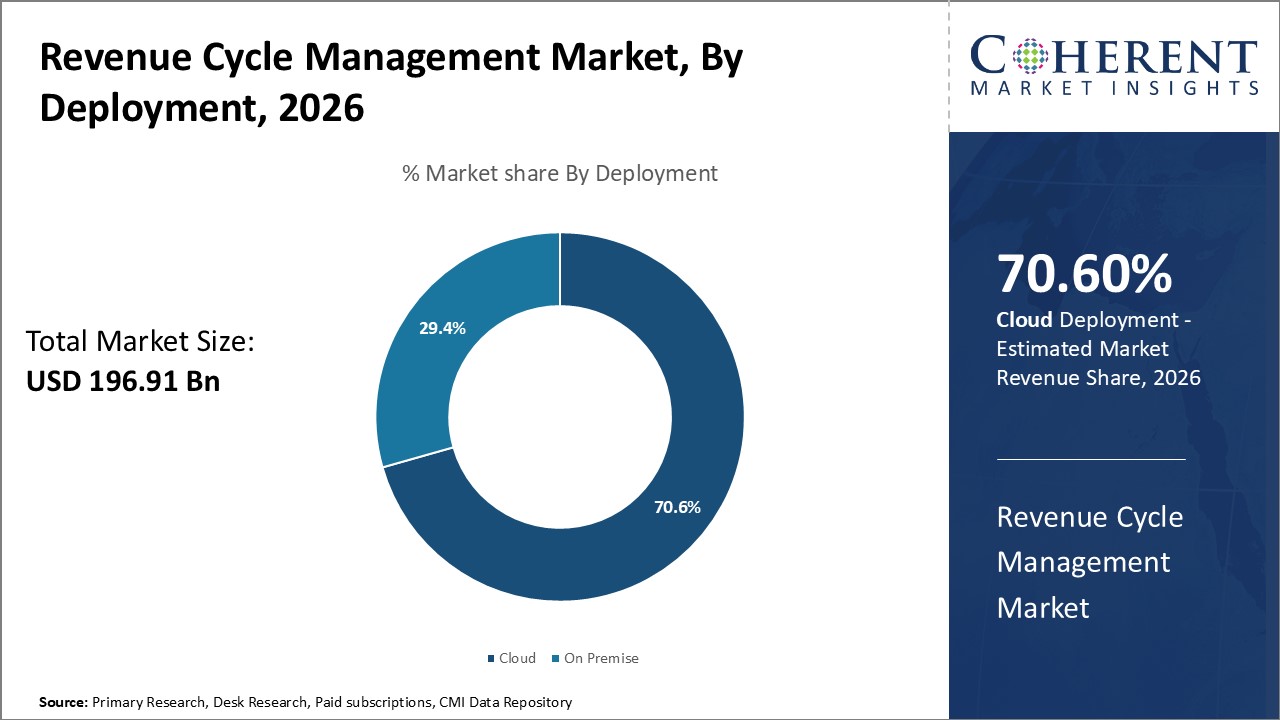
- According to Deployment, The Cloud Segment is anticipated to hold 70.6% share of the Revenue Cycle Management market in 2026. Cloud RCM improves productivity, billing accuracy, and regulatory compliance by utilizing virtualization, artificial intelligence, parallel computing, and real-time analytics.
- According to Component, Software Segment is expected to dominate the revenue cycle management market with 85.3% shares in 2026. The ongoing introduction of cutting-edge solutions targeted at enhancing revenue cycle management in hospitals and medical offices has propelled the software segment to the top of the Revenue Cycle Management Market share.
- According to region, North America holds the largest market share of 40.2% for Revenue Cycle Management market growth by 2026. In this region healthcare companies are being forced to invest in strong RCM systems for compliance and precise revenue capture by laws like HIPAA and the adoption of new coding standards.
Market Overview
The Revenue Cycle Management Market Size is expanding rapidly because to the demand for effective healthcare billing procedures, the shift to value based treatment, and growing regulatory requirements. The market is expected to witness high growth owing to the rising number of healthcare claims and increasing pressure to reduce healthcare costs. With growing digitization of healthcare processes, the demand for automated revenue cycle management solutions is expected to increase. Key players in the market are focusing on offering cloud-based integrated revenue cycle management (RCM) solutions to provide improved workflow, maximize revenue recovery, and enhance patient experience.
Current Events and Its Impact on the Revenue Cycle Management Market
|
Event |
Description and Impact |
|
AI and Automation Adoption |
|
|
National Digital Health Initiatives |
|
Uncover macros and micros vetted on 75+ parameters: Get instant access to report
Pricing Analysis
- Pricing in the Revenue Cycle Management market generally takes the form of software licensing, implementation, subscription fees, or revenue-sharing arrangements. Costs may be structured as a percentage of collections, or as flat-rate software-as-a-service (SaaS) subscriptions.
- For example, a mid-sized hospital may pay 5% of its monthly collections to an outsourced RCM partner, translating to $50,000 for every $1 million in collected patient revenue. Alternatively, a healthcare organization might subscribe to a cloud-based RCM platform for $10,000–$30,000 annually, depending on features and scale.
- Larger institutions with complex requirements may incur additional costs for integration, training, and ongoing support, which can add another 10%–15% of the initial deployment cost.
- These pricing models reflect the value of streamlined revenue operations versus the costs of traditional in-house processes and are influenced by the size, specialty, and specific needs of the healthcare provider.
Consumer Survey, Feedback, and Unmet Needs
Surveys and feedback in the Revenue Cycle Management (RCM) market highlight persistent pain points for healthcare providers and patients alike. A growing share of users seek greater automation, error-free billing, and streamlined claims processing, but surveys reveal unmet needs in areas such as data integration, real-time transparency, and intuitive user experiences.
Many healthcare organizations identify gaps in interoperability between RCM software and electronic health records (EHRs), leading to delayed or denied claims and increased administrative burden.
Additionally, patients often express frustration about billing clarity and the lack of accessible digital payment solutions, underscoring a demand for more patient-centric RCM features. The need for solutions that enhance administrative efficiency without compromising on compliance and data security remains a top priority, evidenced by continued demand for innovation and new entrants promising to address these challenges.
Revenue Cycle Management Market Insights, By Type
Type segment is sub-segmented into standalone and integrated. Integrated segment is anticipated to hold 59.7% of the market share in 2026. Integrated revenue cycle management platforms consolidate key functions such as patient access, billing, and payment posting into a single interconnected system. This unified approach streamlines workflows, reduces manual handoffs, and provides a holistic view of the revenue cycle in real-time.
By integrating disparate systems and databases, integrated RCM solutions eliminate data redundancy and reconcile information automatically across different stages. This brings significant cost savings through economies of scale by reducing administrative overhead and headcount needed for repetitive reconciliation tasks. It also improves billing accuracy since charges are processed, coded, and transmitted seamlessly within the same environment.
As patient volumes and service lines increase, additional modules and users can be added to the core system with relative ease. This flexibility supports long term growth plans of provider organizations. Integrated RCM also eases regulatory compliance as integrated clinical and financial data enables end-to-end audit trails and compliance with changing reimbursement rules.
To learn more about this report, Request Free Sample
Revenue Cycle Management Market Insights, By Deployment
Deployment segment is sub-segmented into cloud and on premise. The cloud segment is estimated to contribute the highest share of the revenue cycle management market and is projected to hold 70.6% of the market share in 2026. A majority of new revenue cycle implementations today are cloud-native given widespread high-speed internet connectivity and evolving regulatory support for data hosting in collaborative third party environments.
Cloud models eliminate infrastructure expenses related to hardware, servers, maintenance and regular software upgrades which traditionally created high barriers for smaller practices to invest in on-premise systems. Transitioning Capital Expenditure to an Operational Expenditure model via software-as-a-service makes technology investment progressively affordable. Advanced cloud platforms also harness the benefits of virtualization, parallel processing, and artificial intelligence to drive unparalleled analytics capabilities.
Real-time business intelligence dashboards equipped with powerful search tools and configurable workflows elevate user experience on the cloud. Integration of cloud-based RCM systems with third party applications spanning patient engagement, practice management and telehealth further augments care coordination.
Revenue Cycle Management Market Insights, By Component
Component segment is sub-segmented into software and service. Software segment is estimated to contribute the highest share of the revenue cycle management market and is projected to hold 85.3% of the market share in 2026. Advanced artificial intelligence driven coding algorithms and clinical documentation improvement modules embedded in RCM software not only enhance revenue capture but also optimize the revenue cycle itself.
Powerful charge description master management, contract management, and claims processing engines streamline financial operations. Integrated electronic remittance advice and electronic funds transfer further accelerate cash posting and reconciliation. Sophisticated rules engines at the core of leading RCM software allow clients to model revenue cycle specific scenarios, payment validations, denial management routines as well as exception handling protocols without writing code.
Templatized interfaces accelerate onboarding of health plans and facilities while also expediting updates across the board as policies evolve. Configurable compliance checks and auditing rules empower self-audits and proactive issue resolution.
Revenue Cycle Management Market Insights, By Function
Function segment is sub-segmented into Appointment Scheduling, Claims & Denial Management, Medical Coding & Billing, Network Management, and Others. The Claims & Denial Management segment is estimated to contribute the highest share of the revenue cycle management market in 2026. In the Revenue Cycle Management (RCM) market, both internationally and in Europe, the Claims & Denial Management sector is the top function. The rising volume and complexity of medical claims, expanding regulatory requirements, and the high financial risk of claim denials are all directly responsible for this domination.
Rejected claims and the weight of administrative work put providers under increasing strain, slowing reimbursements and causing significant revenue losses. Research shows that over 40% of providers lose more than half a million dollars a year as a result of claim denials, with some losing more than a million dollars annually.
Revenue Cycle Management Market Insights, By End User
End User segment is sub-segmented into cloud and on premise. The cloud segment is estimated to contribute the highest share of the revenue cycle management market in 2026. One of the largest and fastest-growing segments of the revenue cycle management (RCM) market is hospitals.
In order to optimize patient income and expedite collection processes, hospitals must implement advanced RCM solutions in response to a growing number of difficulties, including the complexity of healthcare delivery, rising treatment costs, frequent claim denials, and increased administrative constraints. Large hospitals handling high patient numbers and intricate reimbursement situations need to improve billing accuracy and optimize procedures by integrating Electronic Health Records (EHR) with RCM systems.
Regional Insights
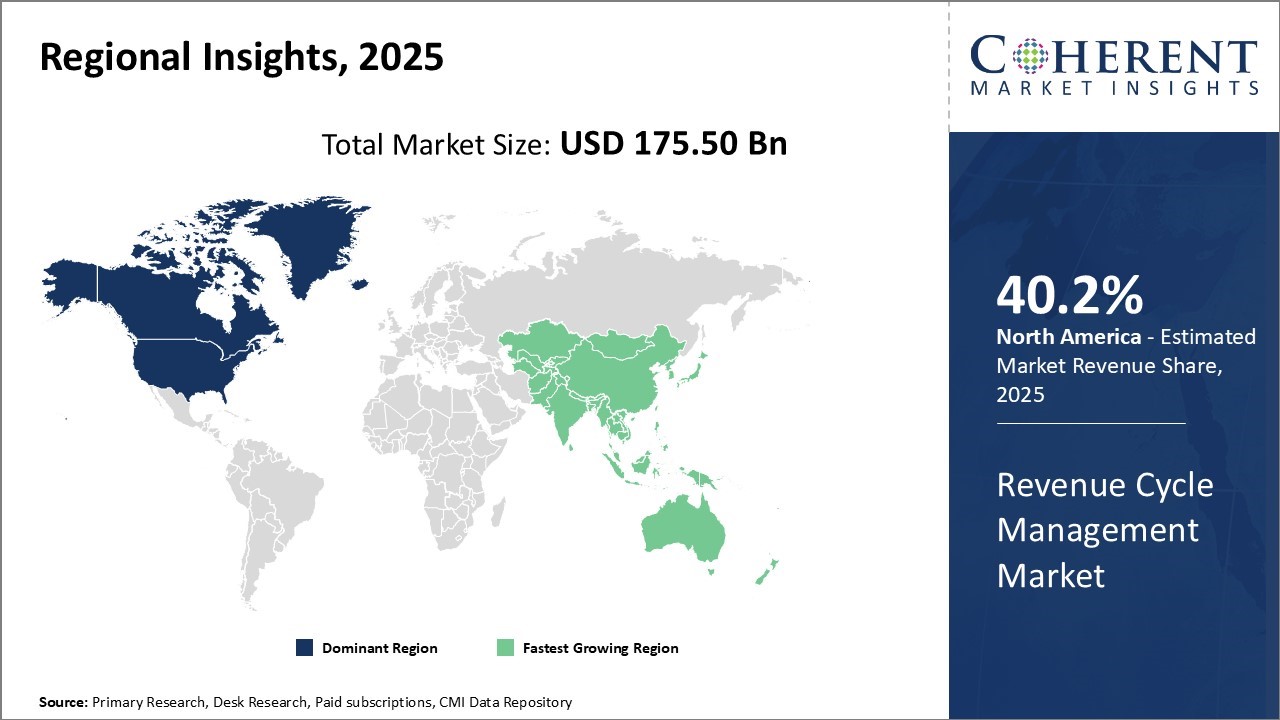
To learn more about this report, Request Free Sample
North America Revenue Cycle Management Market
North America has established itself as the dominant region in the global revenue cycle management market and is anticipated to hold 40.2% of the market share in 2026. The presence of major RCM solution providers and various initiatives taken by healthcare organizations and the government are helping drive significant growth.
The U.S. accounts for the largest share due to high healthcare spending and presence of advanced healthcare IT infrastructure. Many hospitals and physicians' offices are adopting RCM solutions to improve efficiency and cash flows. Moreover, favorable regulations such as the HITECH Act have incentivized the adoption of digital solutions.
Asia Pacific Revenue Cycle Management Market
Asia Pacific is considered as the fastest growing regional market. Rapid economic development, rising medical tourism, and improvements in the healthcare infrastructure across countries like India, China, and Japan are fueling Revenue Cycle Management Market growth opportunities.
With growing concerns around rising healthcare costs, governments and private players are promoting efficient revenue management practices. This has resulted in greater integration of RCM solutions across the vastly expanding Asia Pacific healthcare industry. The growing geriatric population base needing long-term care is another key factor spurring adoption of RCM solutions.
Revenue Cycle Management Market In Europe
Due to the extensive use of technology in healthcare, Germany is the market leader in Europe for RCM, followed by other important markets like the UK and France. Revenue Cycle Management Market with EHR Integration is also gaining momentum, enhancing interoperability and streamlining workflows across clinical and administrative systems.
Cloud-based solutions, robotic process automation, and artificial intelligence are all being used by integrated RCM platforms to improve financial performance, compliance, and billing accuracy.
Revenue Cycle Management Market Dominating Countries
U.S Revenue Cycle Management Market
Utilizing advancements in automation, artificial intelligence, and regulatory compliance, industry titans like Change Healthcare, Epic Systems, McKesson, and Oracle offer complete end-to-end RCM solutions to satisfy the intricate requirements of healthcare providers.
India Revenue Cycle Management Market
The growing patient base, the use of digital health records, and government efforts to digitize healthcare infrastructure are all driving India's RCM market, which is still smaller than the US market. Effective RCM is becoming more and more important to Indian healthcare providers as they deal with issues including billing problems, claim denials, and growing administrative expenses.
Revenue Cycle Management Market In China
Rapid urbanization, significant investment in health IT, and government-led healthcare reforms are all contributing to China's RCM market's strong growth. Advanced RCM platforms are becoming more and more necessary as clinics and hospitals increase patient numbers and service delivery in order to handle intricate reimbursement procedures and expedite patient billing.
Market Report Scope
Revenue Cycle Management Market Report Coverage
| Report Coverage | Details | ||
|---|---|---|---|
| Base Year: | 2025 | Market Size in 2026: | USD 196.91 Bn |
| Historical Data for: | 2020 To 2024 | Forecast Period: | 2026 To 2033 |
| Forecast Period 2026 to 2033 CAGR: | 12.2% | 2033 Value Projection: | USD 440.78 Bn |
| Geographies covered: |
|
||
| Segments covered: |
|
||
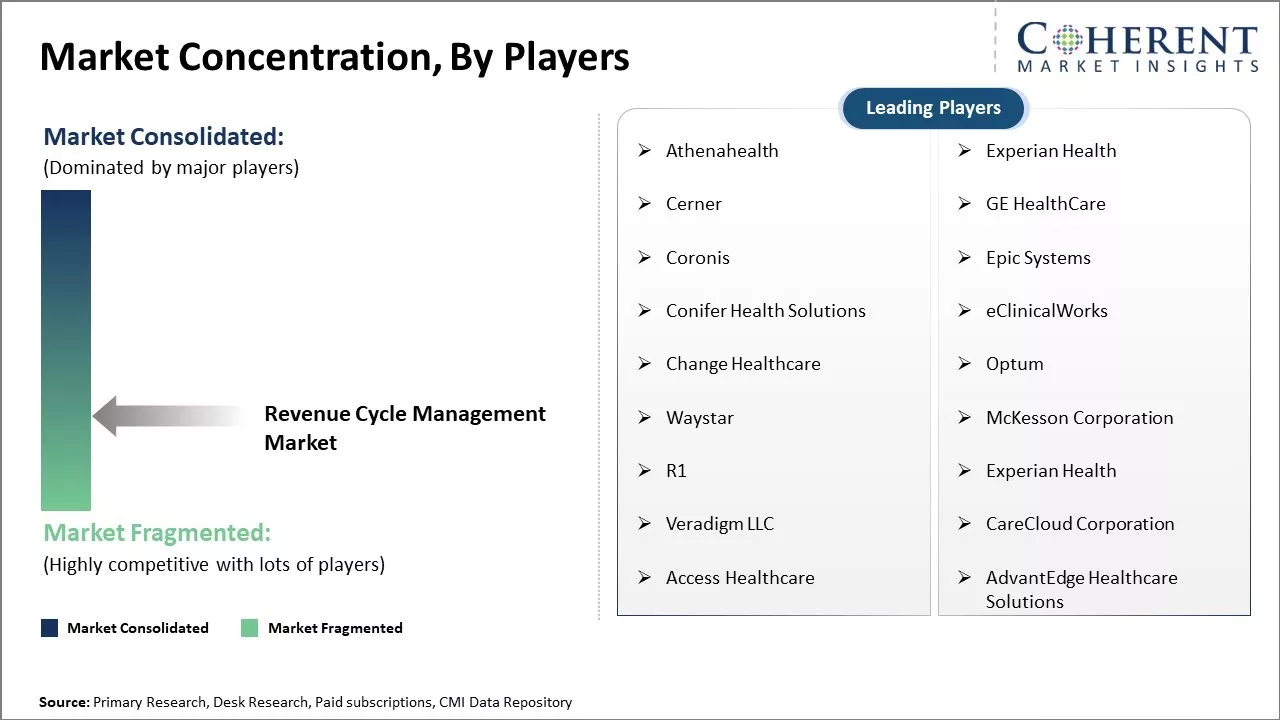
| Companies covered: |
Athenahealth, Experian Health, Cerner, GE HealthCare, Coronis, Epic Systems, Conifer Health Solutions, eClinicalWorks, Change Healthcare, Optum, Waystar, McKesson Corporation, R1, Experian Health, Veradigm LLC, CareCloud Corporation, Access Healthcare, and AdvantEdge Healthcare Solutions |
||
| Growth Drivers: |
|
||
| Restraints & Challenges: |
|
||
Uncover macros and micros vetted on 75+ parameters: Get instant access to report
Revenue Cycle Management Market: Growth Drivers
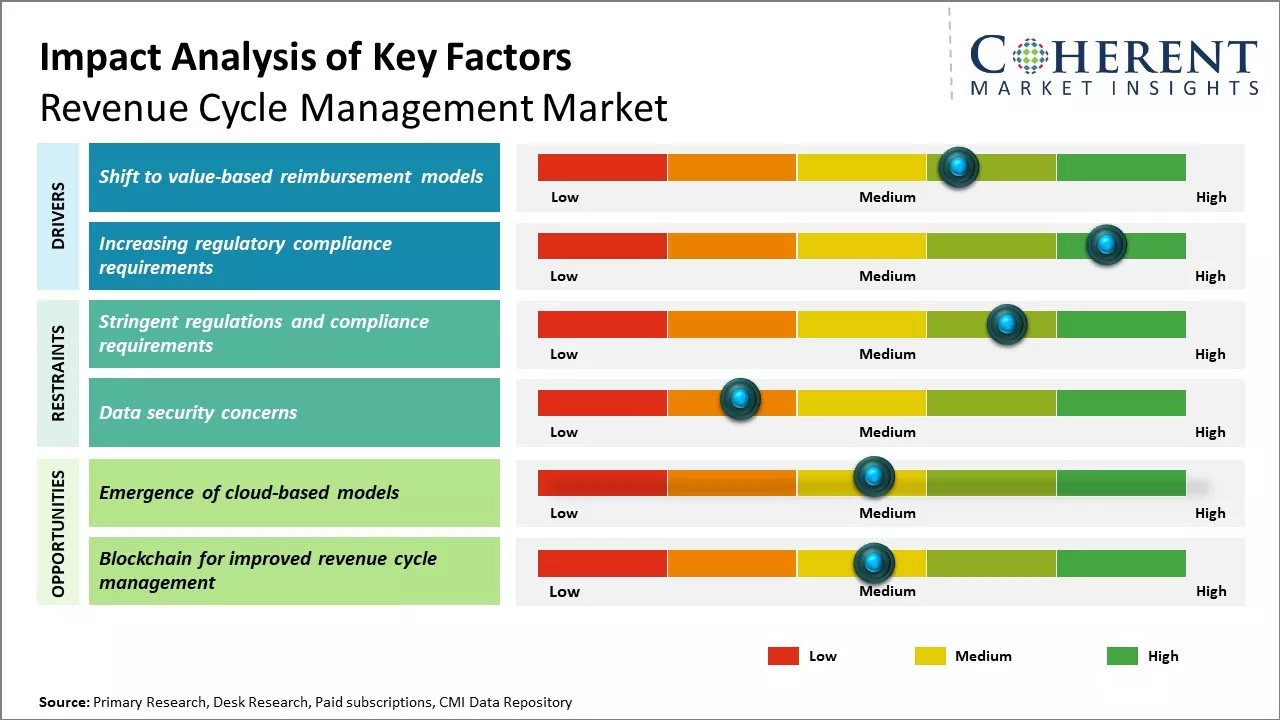
- Shift to value-based reimbursement models
As healthcare costs continue to rise and insurance companies seek to rein in expenses, there is a gradual shift away from fee-for-service models towards value-based healthcare reimbursement models. These newer models tie hospital and provider reimbursements to the overall quality and efficiency of care rather than just sheer volume. This is putting pressure on providers to optimize their revenue cycle processes to minimize billing errors, denials, payment delays, and bad debts.
Revenue cycle management solutions help providers extract maximum reimbursements from payers by ensuring flawless claims submission, denials management, and efficient payment posting. These solutions help providers stay on top of intricate reimbursement rules and regulations so they comply with value-based programs and optimize revenues from both private and public payers. The transition to bundles and episodic payments also increases the need for RCM tools that can track performance across the entire patient encounter.
- Increasing regulatory compliance requirements
Healthcare regulations in the U.S. are becoming more and more complex each year with rules around billing codes, eligibility checks, timely filing, Electronic Remittance Advice/Explanations of Payment (ERA/EOP) compliance, etc. Staying on top of this regulatory maze is challenging for most providers. Non-compliance can result in denied claims, penalties, and audits.
At the same time, the root issue of rising healthcare costs is forcing the government to tighten oversight on revenues and wasteful spending. To address fraudulent and abusive billing practices, agencies like CMS, OIG, and ONC are empowering patients with tools to verify bills and dispute inaccurate charges.
Revenue cycle solutions automate frequently changing rulesets so billing happens flawlessly the first time without errors or rebilling. They help providers integrate with various payer clearinghouses, submit standardized transactions, and address issues pre-emptively before audits. With regulations showing no signs of slowing down, optimization of the revenue cycle is important for hospitals to remain compliant and face less scrutiny from regulatory bodies.
Revenue Cycle Management Market: Restraints
- Stringent regulations and compliance requirements
The revenue cycle management market faces several challenges. Hospitals and healthcare providers struggle with inefficient and outdated revenue cycle processes, leading to losses in potential revenue. Stringent regulations and compliance requirements add complexity that traditional systems have difficulty addressing.
Security of patient health information is also a major concern, as more data is digital but cyber threats continue to evolve. Care teams have less time dedicated to revenue-generating activities as administrative workload rises. New payment models will require agile systems to track performance and enable value-based reimbursement.
- Revenue Cycle Management Market: Trends
Robotic process automation (RPA) is being widely used for data entry, appointment scheduling, insurance verification, and payment posting, freeing staff from repetitive manual tasks. Hospital executives and finance leaders are prioritizing end-to-end RCM platforms over point solutions, while also focusing on enhancing data security to safeguard sensitive patient and billing information.
As reimbursement rates lag behind rising healthcare costs, maximizing revenue through optimized claim capture, improved documentation practices, and denial prevention is more critical than ever. There is also a shift toward solutions that enhance patient access and price transparency, reflecting growing consumer expectations.
Revenue Cycle Management Market: Opportunities
- Emergence of cloud-based models
Cloud-based RCM solutions allow for flexibility and scalability as service capacity can be increased or instantiated rapidly without major investments in new infrastructure. Revenue cycle management of prior authorization is one such area that benefits significantly from this approach, as automated solutions streamline approvals, reduce delays, and improve patient access to care. This enables organizations to adapt quickly to changing market dynamics and scale processes up or down as needed.
The cloud model also reduces upfront capital costs since infrastructure is sourced on-demand and costs are operationalized. This makes cloud RCM affordable for even small and medium sized healthcare facilities. Importantly, cloud solutions ensure 24/7 access to RCM systems from any location via an internet connection. This supports distributed and remote workforces as well as telehealth services that have grown rapidly during the pandemic.
Revenue Cycle Management Market: Key Developments
- July 2025, Omega Healthcare, announced an expanded collaboration with Microsoft. In order to improve the revenue cycle operations and financial performance of healthcare organizations, Omega Healthcare has introduced over 20 generative and agentic AI solutions through the integration of Microsoft Azure's state-of-the-art AI models via Azure AI Foundry and the company's proprietary Omega Digital Platform (ODP).
- May 2025, New Mountain Capital is making its largest platform investment to date targeting the healthcare revenue cycle management space. A new company, called Smarter Technologies, launched combining three health tech companies backed by the private equity firm Access Healthcare, Thoughtful.ai and SmarterDx.
Analyst Opinion
- The market growth is propelled by the continued digitization of healthcare, rising volumes of healthcare claims, and a heightened focus on cost containment and operational efficiency.
- The shift from fee-for-service to value-based reimbursement models is a decisive trend, pushing healthcare providers to adopt sophisticated RCM solutions to optimize revenue, minimize claim denials, and comply with evolving regulatory requirements.
- Rapid technological adoption such as AI, automation, and integrated cloud-based systems as key levers improving workflow, financial visibility, and patient experience.
- The pressing need for integrated platforms that manage clinical and financial data, alongside regulatory mandates like EHR adoption, is accelerating market momentum.
Market Segmentation
- By Type (Revenue, USD Bn, 2021 - 2033)
-
- Standalone
- Integrated
- By Deployment (Revenue, USD Bn, 2021 - 2033)
-
- Cloud
- On Premise
- By Component (Revenue, USD Bn, 2021 - 2033)
-
- Software
- Service
- By Function (Revenue, USD Bn, 2021 - 2033)
-
- Appointment Scheduling
- Claims & Denial Management
- Medical Coding & Billing
- Network Management
- Others
- By End User (Revenue, USD Bn, 2021 - 2033)
-
- Hospitals
- Clinics
- Ambulatory Surgical Centres
- Diagnostics & Imaging Centres
- Others
Regional Insights (Revenue, USD Bn, 2021 - 2033)
- North America
- U.S.
- Canada
- Latin America
- Brazil
- Argentina
- Mexico
- Rest of Latin America
- Europe
- Germany
- U.K.
- Spain
- France
- Italy
- Russia
- Rest of Europe
- Asia Pacific
- China
- India
- Japan
- Australia
- South Korea
- ASEAN
- Rest of Asia Pacific
- Middle East
- GCC Countries
- Israel
- Rest of Middle East
- Africa
- South Africa
- North Africa
- Central Africa
- North America
- Company Profiles
-
- Athenahealth
- Experian Health
- Cerner
- GE HealthCare
- Coronis
- Epic Systems
- Conifer Health Solutions
- eClinicalWorks
- Change Healthcare
- Optum
- Waystar
- McKesson Corporation
- R1
- Experian Health
- Veradigm LLC
- CareCloud Corporation
- Access Healthcare
- AdvantEdge Healthcare Solutions
Sources
Primary Research Interviews
- Healthcare IT Consultants
- RCM Software Product Managers
- Third-party Medical Billing Service Providers
- Healthcare Compliance Officers
Databases
- Embase
- EEE Xplore
- SpringerLink
- ClinicalKey
Magazines
- Revenue Cycle Advisor
- Becker’s Hospital Review (Magazine format)
- Managed Healthcare Executive
- For The Record
Journals
- Journal of Revenue and Pricing Management
- American Journal of Managed Care
- Journal of Biomedical Informatics
- Healthcare Financial Management Journal
Newspapers
- The Economic Times (Healthcare/Industry)
- Business Standard (Healthcare Segment)
- Financial Times (Healthcare Insights)
- The Hindu Business Line (Health & Pharma)
Associations
- Healthcare Information and Management Systems Society (HIMSS)
- American Hospital Association (AHA)
- Workgroup for Electronic Data Interchange (WEDI)
- National Association of Healthcare Access Management (NAHAM)
- American Academy of Professional Coders (AAPC)
- Centers for Medicare & Medicaid Services (CMS)
Proprietary Elements
- CMI Data Analytics Tool, Proprietary CMI Existing Repository of information for last 8 years
*Definition: The revenue cycle management market consists of software, services, and platforms that help healthcare organizations efficiently manage the complex billing and payment processes associated with patient care. It covers tasks from patient registration through claims adjudication, billing, and follow-up. The goal is to streamline revenue generation from payers while improving affordability for patients. Revenue cycle management solutions help providers collect payments faster, reduce denials and administrative costs, and improve the patient financial experience.
Share
Share
About Author
Komal Dighe is a Management Consultant with over 8 years of experience in market research and consulting. She excels in managing and delivering high-quality insights and solutions in Health-tech Consulting reports. Her expertise encompasses conducting both primary and secondary research, effectively addressing client requirements, and excelling in market estimation and forecast. Her comprehensive approach ensures that clients receive thorough and accurate analyses, enabling them to make informed decisions and capitalize on market opportunities.
Missing comfort of reading report in your local language? Find your preferred language :
Transform your Strategy with Exclusive Trending Reports :
Frequently Asked Questions
EXISTING CLIENTELE
Joining thousands of companies around the world committed to making the Excellent Business Solutions.
View All Our Clients