Medical Claims Processing Services Market Size and Forecast – 2026 – 2033
The Global Medical Claims Processing Services Market size is estimated to be valued at USD 14.6 billion in 2026 and is expected to reach USD 27.9 billion by 2033, exhibiting a compound annual growth rate (CAGR) of 10.3% from 2026 to 2033.
Global Medical Claims Processing Services Market Overview
Medical claims processing services involve specialized platforms and services that manage the submission, validation, adjudication, and reimbursement of healthcare insurance claims. These products include automated claims management software, coding and billing tools, compliance verification systems, and analytics dashboards. The services help healthcare providers and insurers reduce errors, accelerate reimbursement cycles, and ensure adherence to regulatory and payer requirements. They are widely used by hospitals, clinics, insurance companies, and third-party administrators.
Key Takeaways
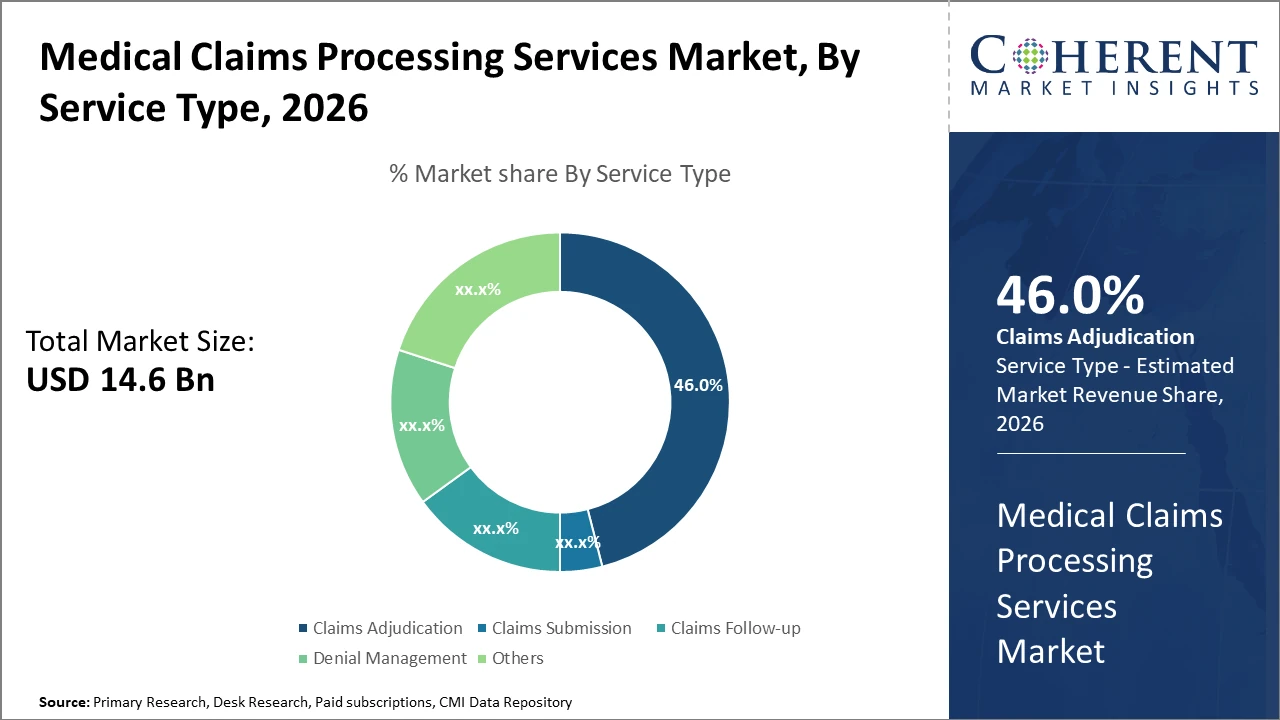
Claims Adjudication dominates the service type segment, holding 46% market share, reflecting the critical importance of accurate claims validation. Claims Follow-up is emerging as the fastest-growing subsegment driven by its role in enhancing reimbursement rates.
Hospitals and Healthcare Providers command the largest market share in the end-user segment, underscoring the direct impact of claims services on healthcare facilities’ revenue cycle health, while Government Healthcare Programs are rapidly adopting automated processing in emerging economies.
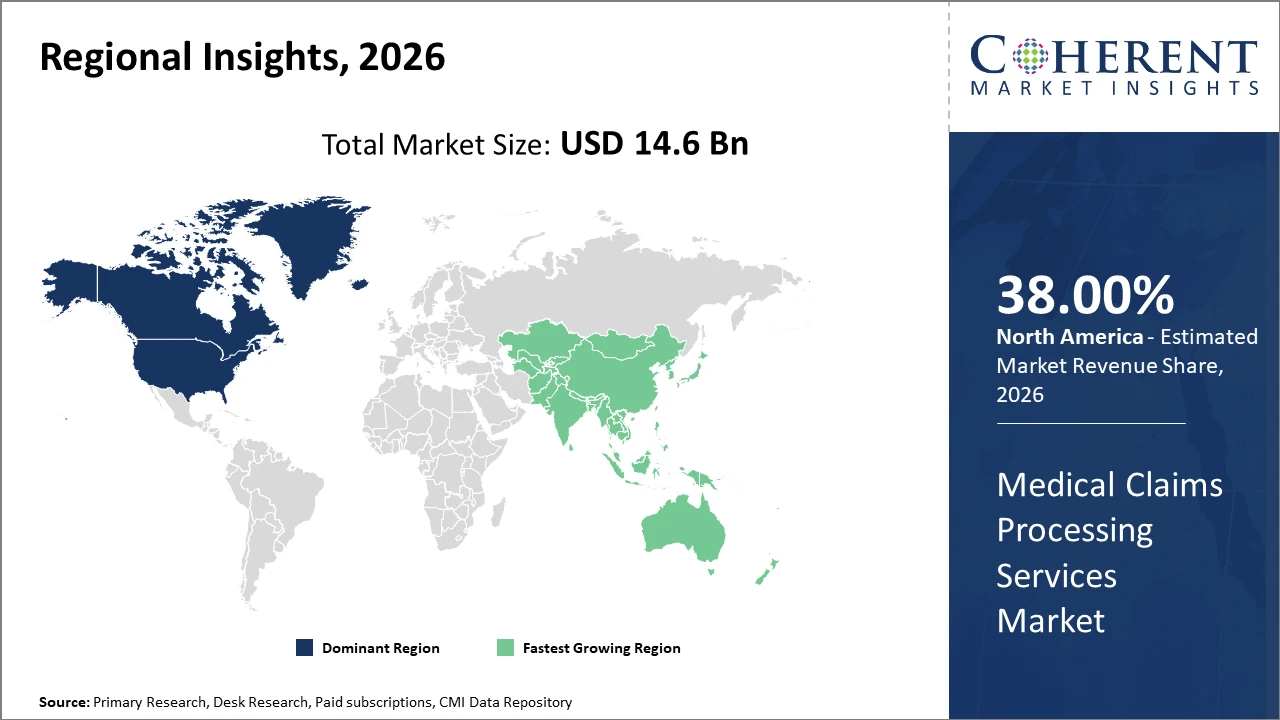
North America leads regional market share at 38%, driven by mature insurer frameworks and regulatory mandates, while Asia Pacific is the fastest-growing region due to expanding healthcare infrastructure and rising insurance penetration.
Cloud-based deployment models are gaining significant traction, capturing over 35% of market revenue by 2026, indicating a strategic shift towards scalable and remote service delivery.
Medical Claims Processing Services Market Segmentation Analysis
To learn more about this report, Request Free Sample
Medical Claims Processing Services Market Insights, By Service Type
Claims Adjudication dominates the market share with 46%. This subsegment benefits from stringent regulations requiring precise claims verification before payments, thus ensuring compliance and revenue accuracy. It involves activities such as eligibility verification and claim validation, which are critical for reducing claim denials and accelerating reimbursements. Claims Follow-up is the fastest-growing subsegment, driven by increasing complexities in claims resubmission processes and the need to capture delayed payments. This service enhances recovery rates by ensuring claims initially rejected or pending are systematically managed.
Medical Claims Processing Services Market Insights, By End-User
Hospitals and Healthcare Providers hold the largest share. They require efficient claims processing to maintain revenue cycles, given the high volume of patient billing. Investment in integrated claims processing platforms has shown a direct correlation with improved Days in Accounts Receivable (AR) metrics, as reported by leading hospital systems in 2024. Government Healthcare Programs are experiencing the fastest growth, particularly in emerging regions, due to increased public healthcare funding and insurance enrollment expansions. Insurance Companies rely heavily on claims processing services to validate claims and control fraud. TPAs focus on intermediary claims management, growing steadily as outsourced services increase.
Medical Claims Processing Services Market Insights, By Deployment Mode
Cloud-based deployment is the fastest-growing segment, favored for its scalability, cost-efficiency, and ease of updates. Cloud-based claims processing solutions grew by over 35% in adoption rates in 2024, as providers and payers sought agile platforms amid rising claim volumes and regulatory complexities. Hybrid models, combining on-premise control with cloud flexibility, are gaining traction as transitional solutions. On-premise installations remain pertinent where data sovereignty laws are strict or where organizations prefer localized control. Other deployment models include managed services and software-as-a-service (SaaS) variants tailored to smaller providers or bespoke use cases.
Medical Claims Processing Services Market Trends
Medical claims processing services are witnessing accelerated digital transformation driven by AI, blockchain, and cloud integration.
For example, in 2025, over 60% of claims service providers globally integrated AI-based fraud detection, substantially lowering erroneous payments.
Blockchain pilots in Europe in 2024 highlighted a 15% improvement in claims reconciliation accuracy.
Another trend is the growing importance of value-based care models merging clinical and claims data, particularly in North America, which has caused shifts in service offerings geared towards performance-based reimbursements.
Medical Claims Processing Services Market Insights, By Geography
To learn more about this report, Request Free Sample
North America Medical Claims Processing Services Market Analysis and Trends
In North America, the dominance in the Medical Claims Processing Services market is grounded in high healthcare expenditures, robust insurer networks, and stringent regulatory frameworks such as HIPAA, driving the adoption of advanced claims processing solutions. U.S. market players contribute nearly 38% to the market share, leveraging cutting-edge technologies to streamline claims workflows.
Asia Pacific Medical Claims Processing Services Market Analysis and Trends
Meanwhile, the Asia Pacific exhibits the fastest growth with a CAGR of 12%, attributed to healthcare infrastructure expansion, increased insurance coverage, and government initiatives promoting digital health services. Countries like India and China are notable contributors, benefitting from increasing demand for streamlined claims management.
Medical Claims Processing Services Market Outlook for Key Countries
USA Medical Claims Processing Services Market Analysis and Trends
The USA's market is pivotal, accounting for over one-third of the total market revenue. Increasing focus on compliance with regulatory mandates and accelerated AI adoption has been central to business growth. Major Medicaid and Medicare reforms in 2024 prompted greater demand for cloud-based adjudication systems. Leading companies, such as Optum and Cognizant, have heavily invested in service automation and analytics, driving enhanced claim accuracy and faster reimbursements.
India Medical Claims Processing Services Market Analysis and Trends
India’s market is rapidly expanding, fueled by government schemes such as Ayushman Bharat, which have boosted insurance penetration and volumes of processed claims. Local providers are partnering with global companies to implement AI and cloud-based platforms. This has driven market revenue growth, as digitalization efforts facilitate improved claim cycle management for a vast patient base across both urban and rural areas.
Analyst Opinion
Increasing Integration of AI and Automation: The introduction of AI-powered tools and robotic process automation (RPA) in medical claims processing has significantly boosted operational efficiency and decreased processing errors. For instance, in 2024, industry-wide adoption of AI mechanisms led to an average reduction in claim processing time by over 30%, translating into faster reimbursements and improved cash flow. Large payer organizations reported that automation contributed to a 24% reduction in manual intervention, underscoring its impact on market share growth.
Demand Surge from Emerging Healthcare Markets: Regions such as the Asia Pacific have seen a 15% year-over-year increase in demand for medical claims processing services, fueled by expanding healthcare infrastructure and rising insurance enrolments. This demand amplifies market revenue and drives capacity expansions, with multi-national health plans expanding their footprint in countries like India and China in 2025 to manage burgeoning claim volumes effectively.
Stringent Regulatory Compliance and Data Security: Compliance with HIPAA in the U.S. and GDPR in Europe has spurred investments in secure cloud-based platforms for claims processing. Real-world data from 2024 suggests that 78% of enterprises upgraded to advanced compliance frameworks, catalyzing growth in the medical claims processing services market by assuring stakeholders of data privacy and regulatory adherence.
Shift Toward Value-Based Care Models: The transition from fee-for-service to value-based care has increased the complexity of claims adjudication, demanding sophisticated services to validate claims against clinical outcomes. Early 2025 reports show a 12% rise in demand for services capable of integrating clinical data with claims data, driving specialized service niche expansions within the market.
Market Scope
| Report Coverage | Details | ||
|---|---|---|---|
| Base Year: | 2025 | Market Size in 2026: | USD 14.6 billion |
| Historical Data for: | 2020 To 2024 | Forecast Period: | 2026 To 2033 |
| Forecast Period 2026 to 2033 CAGR: | 10.3% | 2033 Value Projection: | USD 27.9 billion |
| Geographies covered: |
|
||
| Segments covered: |
|
||
| Companies covered: | TCS (Tata Consultancy Services), Conduent Incorporated, Wipro Limited, UnitedHealth Group, DXC Technology, Capgemini SE, MedData LLC, NTT DATA Corporation, HCL Technologies Limited, Allscripts Healthcare Solutions | ||
| Growth Drivers: |
|
||
Uncover macros and micros vetted on 75+ parameters: Get instant access to report
Medical Claims Processing Services Market Growth Factors
The increasing digitization of healthcare administration and the quest for operational efficiency remain paramount growth drivers. In 2025 alone, healthcare providers processing over 70% of claims electronically reported improved revenue cycle KPIs. Secondly, rapid adoption of cloud-based services, which accounted for a 35% rise in deployment in 2024, encourages scalable and cost-effective service models. Thirdly, shifting regulatory landscapes have elevated demand for comprehensive compliance-ready claims processing services—evident from a 25% annual growth in compliance-focused service packages. Lastly, the rising number of insured populations globally, particularly in developing economies, has spiked claim volumes significantly.
Medical Claims Processing Services Market Development
In October 2025, Optum launched Optum Real, an AI-backed, real-time communication platform designed to fundamentally streamline interactions between healthcare providers and payers. The system enables clinicians to verify insurance coverage, submit required clinical data, and resolve prior-authorization elements during the patient visit itself, rather than weeks later. By embedding intelligence directly into the point-of-care workflow, Optum Real aims to significantly reduce claim denials, administrative backlogs, and revenue cycle delays while improving transparency and care continuity.
In February 2025, Capital Rx introduced Judi Health™, the industry’s first unified claim processing platform that brings pharmacy and medical claims into a single, integrated workflow. Judi Health addresses long-standing fragmentation in healthcare administration by eliminating silos between benefit types, allowing payers and administrators to manage claims more efficiently, reduce errors, and gain a holistic view of patient utilization and costs across the care continuum.
In late 2024, Oracle Health launched its Clinical Data Exchange, a cloud-based solution designed to automate secure medical record transmission between providers and payers. The platform accelerates the adjudication of complex clinical claims by ensuring timely access to complete and standardized patient data, while maintaining high levels of interoperability, compliance, and data security.
Key Players
Leading Companies of the Market
TCS (Tata Consultancy Services)
Conduent Incorporated
Wipro Limited
UnitedHealth Group
DXC Technology
Capgemini SE
MedData LLC
NTT DATA Corporation
HCL Technologies Limited
Allscripts Healthcare Solutions
Optum, Inc. leveraged AI and analytics to enhance claims accuracy, resulting in a 15% improvement in denial rate reduction in 2024. Cognizant Technology Solutions expanded its footprint through strategic partnerships with regional insurers in Asia Pacific, increasing service adoption by 20% in emerging markets during 2025. EXL Service Holdings implemented blockchain pilot projects to streamline claims verification, reporting a 10% reduction in fraudulent claims processing in its 2024 operations.
Medical Claims Processing Services Market Future Outlook
The medical claims processing services will be transformed by artificial intelligence, machine learning, and robotic process automation (RPA). These technologies will enhance accuracy, detect anomalies, and expedite turnaround times. Natural language processing will improve the interpretation of unstructured clinical documentation, while predictive analytics will support proactive denial management. Blockchain technologies may play a role in secure, transparent claim execution. Interoperability with electronic health records and payer systems will further streamline workflows. As healthcare payment models evolve toward value-based care, claims processing services will need to support complex pricing, bundled payments, and outcome-based reimbursement models.
Medical Claims Processing Services Market Historical Analysis
The medical claims processing services market emerged alongside the growth of health insurance in the 20th century, when paper-based claims and manual adjudication dominated administrative workflows. As healthcare systems expanded and claim volumes increased, inefficiencies, billing errors, and fraud became significant challenges. Early automation efforts introduced electronic data interchange (EDI) standards to streamline information exchange between providers and payers. Over time, claims processing systems incorporated more sophisticated rules engines, compliance auditing, and integration with practice management systems. Outsourced claims processing services grew as providers sought to reduce administrative burdens and accelerate reimbursement.
Sources
Primary Research Interviews:
Revenue cycle managers
insurance administrators
healthcare billing specialists
Databases:
CMS Claims Data
OECD Health Finance Data
World Bank Health Systems Data
HIMSS Analytics
Magazines:
Healthcare Finance News
Revenue Cycle Advisor
Medical Economics
Becker’s Healthcare Finance
Health IT Analytics
Journals:
Journal of Healthcare Management
Health Economics Review
BMC Health Services Research
Journal of Medical Systems
Healthcare Finance Review
Newspapers:
Financial Times (Healthcare)
Reuters Health
The Wall Street Journal (Insurance)
Bloomberg Health
The Guardian (Public Policy)
Associations:
Healthcare Financial Management Association
American Health Information Management Association
Medical Group Management Association
National Association of Healthcare Revenue Integrity
American Hospital Association
Share
Share
Ghanshyam Shrivastava - With over 20 years of experience in the management consulting and research, Ghanshyam Shrivastava serves as a Principal Consultant, bringing extensive expertise in biologics and biosimilars. His primary expertise lies in areas such as market entry and expansion strategy, competitive intelligence, and strategic transformation across diversified portfolio of various drugs used for different therapeutic category and APIs. He excels at identifying key challenges faced by clients and providing robust solutions to enhance their strategic decision-making capabilities. His comprehensive understanding of the market ensures valuable contributions to research reports and business decisions.
Ghanshyam is a sought-after speaker at industry conferences and contributes to various publications on pharma industry.
Joining thousands of companies around the world committed to making the Excellent Business Solutions.
View All Our Clients