U .S. Healthcare Revenue Integrity Market Size and Forecast – 2026 To 2033
The U.S. healthcare revenue integrity market is expected to grow from USD 3,448.8 Mn in 2026 to USD 5,692.5 Mn by 2033, registering a compound annual growth rate (CAGR) of 8.6%. The U.S. healthcare revenue integrity market is steadily expanding, fueled by the increasing intricacies of claims and reimbursement management.
According to the Centers for Medicare & Medicaid Services, Medicare covers over 65 million beneficiaries, making it one of the largest and most complex reimbursement systems in the U.S.
(Source: Centers for Medicare & Medicaid Services)
Key Takeaways of the U.S. Healthcare Revenue Integrity Market
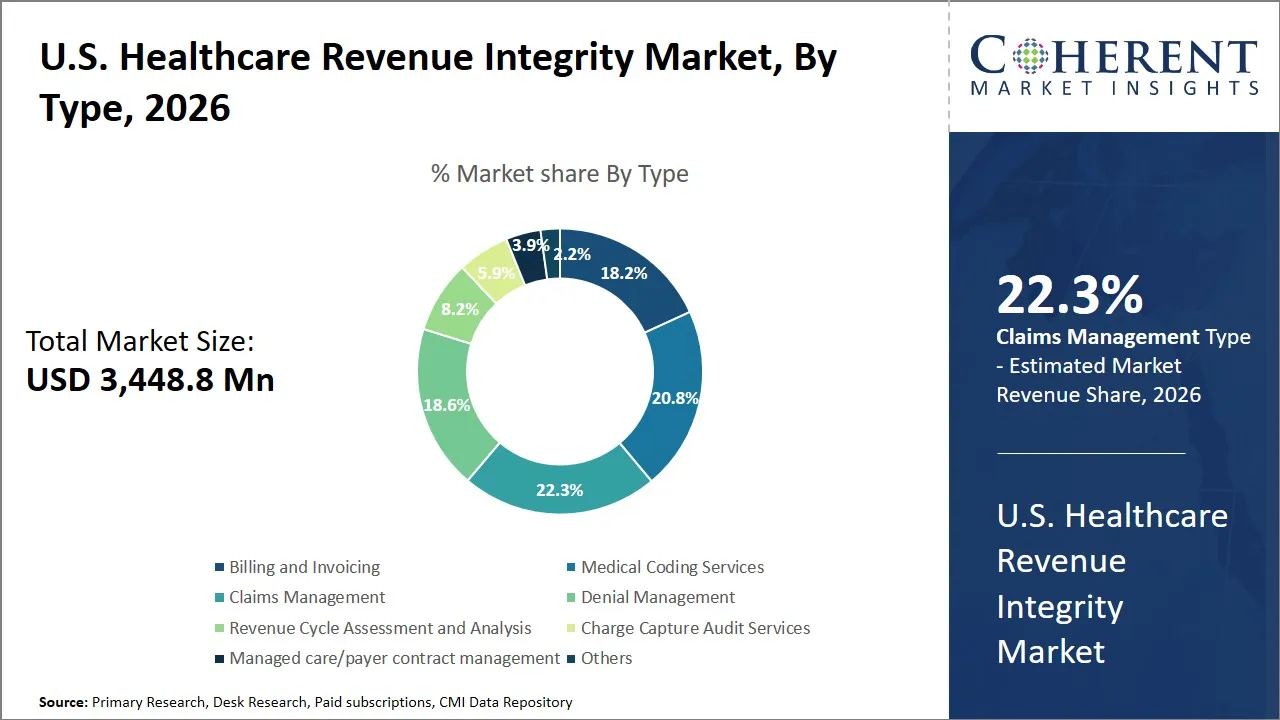
- Claims management is projected to hold 22.3% of the U.S. healthcare revenue integrity market share in 2026, making it the dominant type segment. This is owing to the sheer size and importance associated with billing activities, wherein any small mistake could cause significant losses in terms of revenue generation. As per Centers for Medicare & Medicaid Services (CMS) estimates, improper payments by the Medicare scheme were estimated at about USD 28.83 billion in 2025. (Source: Centers for Medicare & Medicaid Services)
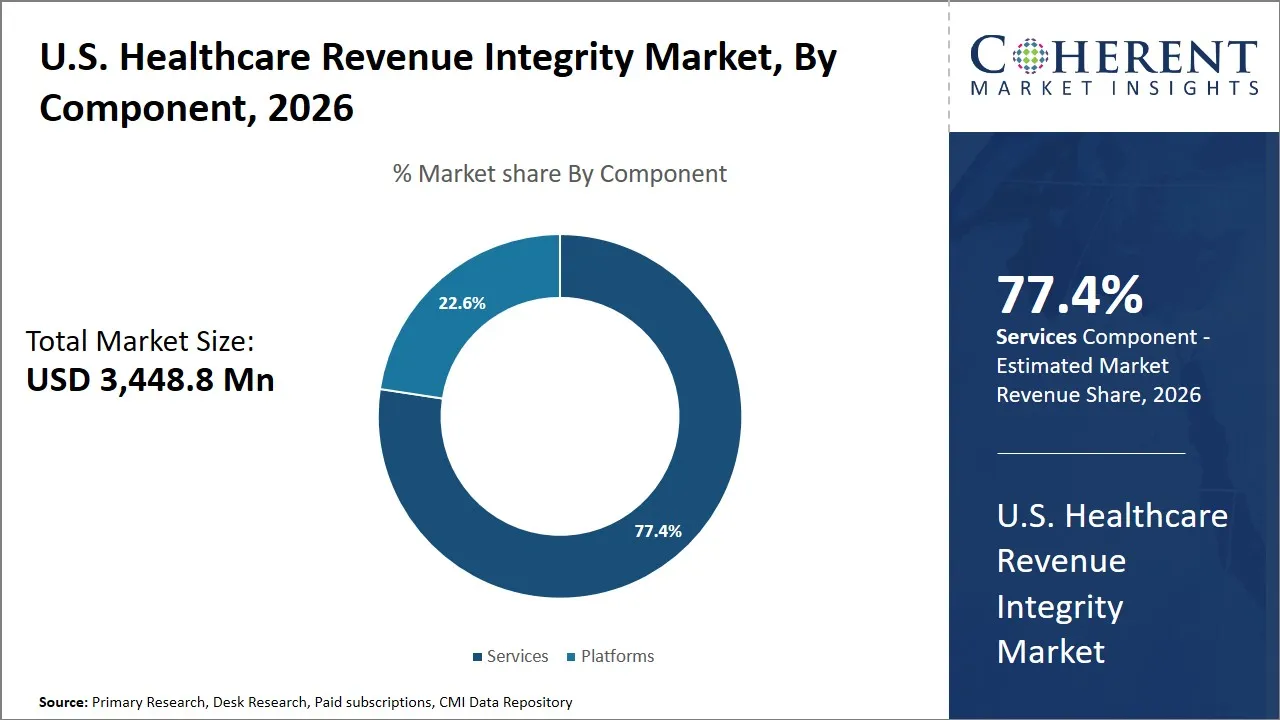
- Services are projected to hold 77.4% of the U.S. healthcare revenue integrity market share in 2026, making it the dominant component segment driven by the surging demand for qualified specialists in coding, managing denials, and complying with federal regulations (e.g., Health Insurance Portability and Accountability Act (HIPAA)). In addition, outsourcing and consultancy services have been gaining popularity in the healthcare industry (about 80% of healthcare organizations utilize outsourcing services for managing revenue cycle processes, data by Auxis). The reasons for such dependence on external sources are the complexity of the reimbursement system, insufficient staff, and operational efficiency of revenue cycle management processes.
- The on-premises sub-segment is projected to hold 50.4% of the U.S. healthcare revenue integrity market share in 2026, making it the dominant deployment model segment. Although there is an increasing trend towards the adoption of cloud-based technology in the healthcare revenue integrity market, on-premise systems continue to be preferred by large healthcare providers. This is due to their ability to offer enhanced control over sensitive patient data, support compliance with stringent regulatory requirements, and enable seamless integration with complex legacy IT infrastructures. Enterprise-scale solutions offered by players such as Epic Systems are often deployed on-premise to ensure customization, system reliability, and long-term operational control, particularly in large hospital networks.
- Integration of Prior Authorization Automation within Revenue Cycle Management (RCM )Systems: Due to the rising complexity of prior authorizations, there is an increasing tendency toward the automation of verification and approval processes through revenue cycle management The integration of prior authorizations with revenue integrity solutions will help decrease delays, avoid claim denials, and facilitate payment procedures.
- Revenue Integrity Solutions for Outpatient & Ambulatory Care Centers: With the increasing shift of care delivery from inpatient hospitals to outpatient and ambulatory care settings, there is a growing need for specialized revenue integrity systems that cater to large numbers of patients, fast turnaround of bills, and varied payers. Such environments typically lack robust RCM capabilities, which creates a gap that needs to be filled by revenue integrity systems.
Why Does the Claims Management Segment Dominate the U.S. Healthcare Revenue Integrity Market?
Claims management is projected to hold a market share of 22.3% in 2026. Claims management is a crucial aspect of the U.S. healthcare revenue integrity market owing to the large number of claims processed and the significant financial risks related to claim denials and operational problems. According to a study by Premier Inc., U.S. health insurers process approximately 3 billion medical claims annually and approximately 70% of denials are overturned and paid highlighting the critical need for efficient claims handling systems. (Source: Premier Inc.)
Furthermore, in May 2024, STAT News reported that nearly 15% of claims are initially denied. This creates a financial strain, costing healthcare providers approximately USD 19.7 billion annually. (Source: STAT News)
Concurrently, industry figures show that between 35% and 60% of denied claims never make it back into the system for reconsideration, leading to significant revenue losses (Source: Aptarro, Inc.). These instances highlight the significant investments healthcare organizations make in advanced claims management systems. The aim is to boost initial acceptance rates, minimize claim denials, and safeguard their financial well-being.
Why are Services the Most Preferred Component in the U.S. Healthcare Revenue Integrity Market?
To learn more about this report, Request Free Sample
Services are projected to hold 77.4% of the market share in 2026. This trend reflects the growing dependence of healthcare providers on specialists to navigate the intricate world of billing, coding, and denial management. To streamline their processes and reduce administrative load, numerous healthcare organizations are now turning to external firms for revenue cycle and integrity functions.
A study at Harvard T.H. Chan School of Public Health and published in Health Affairs reveals that administrative expenses represent about 25%-31% of health care spending in the U.S. (Source: Health Affairs). Moreover, research published in the National Library of Medicine estimates that the U.S. healthcare system spends almost USD 1 trillion each year on administrative tasks, including those related to revenue cycle management. This includes processes such as medical coding, billing, claims submission, payment reconciliation, and denial management (Source: National Library of Medicine). Consequently, the increased expenses and intricacies inherent in healthcare operations necessitate that providers heavily rely on outsourced and managed services. These services offer specialized knowledge, scalability, and enhanced efficiency, thereby solidifying their position as the primary component within the healthcare revenue integrity sector.
On-Premises Segment Dominates the U.S. Healthcare Revenue Integrity Market
The on-premises segment is expected to hold 50.4% of the U.S. healthcare revenue integrity market share in 2026. The growing need for strong security measures, the need to follow complex compliance rules, and the requirement to fully control sensitive Protected Health Information (PHI) are the main reasons for this increase. The healthcare sector's hesitance to adopt cloud computing is underscored by findings from the Cloud Security Alliance. The research indicates that only 47% of vital healthcare information is stored in the cloud, a figure notably lower than the 61% average observed across other industries (Source: Cloud Security Alliance). Moreover, on-premise solutions offer users complete control over sensitive data, including both its storage and the protocols governing access.
Currents Events and their Impact
|
Current Events |
Description and its Impact |
|
Regulatory Shift: Expansion of Value-Based Care Models (2024–2025) |
|
|
Industry Disruption: Change Healthcare Cyberattack Disrupting Revenue Cycle Operations (2024) |
|
Uncover macros and micros vetted on 75+ parameters: Get instant access to report
(Source: Centers for Medicare & Medicaid Services, Centers for Medicare & Medicaid Services)
U.S. Healthcare Revenue Integrity Market Dynamics
To learn more about this report, Request Free Sample
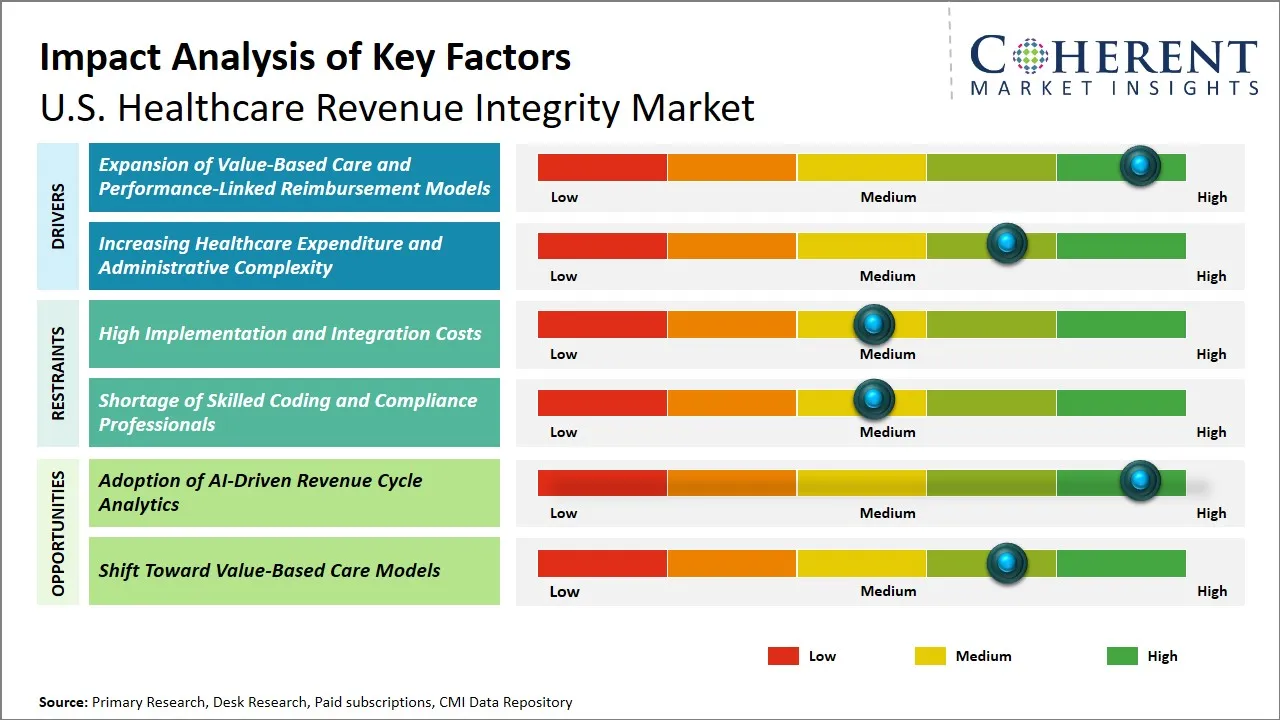
Market Drivers
- Expansion of Value-Based Care and Performance-Linked Reimbursement Models: The growing trend of value-based care (VBC) in the U.S. has led to a surge in the adoption of innovative revenue integrity solutions. In value-based care models, reimbursement is based on the quality, effectiveness, and efficiency of the service delivered. According to Centers for Medicare & Medicaid Services (CMS), the percentage of Traditional Medicare members who participated in accountable care agreements in 2025 was 53.4%. The shift towards a performance-based payment model requires revenue integrity products that improve coding accuracy and maximize payments. (Source: Centers for Medicare & Medicaid Services)
- Increasing Healthcare Expenditure and Administrative Complexity: The rising costs of healthcare in the U.S. is a major factor driving the need for effective revenue integrity solutions. The sheer scale of financial transactions makes billing, coding, and getting paid back a real hustle. The Centers for Medicare & Medicaid Services reported that the U.S. Healthcare expenditures reached USD 4.9 trillion in 2023, accounting for 17.6% of the country's gross domestic product. This increase in spending adds to administrative workloads and the potential for lost revenue. Consequently, healthcare providers are turning to sophisticated revenue integrity systems. These systems are designed to ensure precise claims management, adherence to regulations, and the best possible financial outcomes. (Source: Centers for Medicare & Medicaid Services)
Emerging Trends
- Adoption of AI-Driven Revenue Integrity Solutions: The applications of AI and ML are currently being used in the field of healthcare to verify coding, predict claim denials, and prevent revenue leakage in a proactive manner rather than a reactive way of handling the revenue cycle management process.
- Shift Toward Autonomous and Cloud-Based RCM Platforms: The healthcare industry is experiencing rapid implementation of autonomous revenue cycle management tools because they can integrate seamlessly into the Electronic Health Records (EHR) and are scalable and interoperable throughout the health network.
Regulatory & Reimbursement Landscape Shaping the U.S. Healthcare Revenue Integrity Market
|
Category
|
Regulation |
Key Details |
Impact on Revenue Integrity |
|
Coding & Billing Standards |
Centers for Medicare & Medicaid Services – ICD-10-CM/PCS |
Mandatory use of standardized coding systems with strict documentation requirements for claims submission |
Drives demand for coding accuracy, audit, and compliance solutions |
|
Value-Based Reimbursement |
Centers for Medicare & Medicaid Services – Quality Payment Program (QPP) |
Reimbursement linked to quality, cost efficiency, and performance metrics |
Increases need for analytics-driven revenue integrity and performance tracking |
|
Billing Transparency Regulation |
U.S. Department of Health and Human Services – No Surprises Act |
Requires transparent billing, accurate estimates, and dispute resolution for unexpected medical bills |
Strengthens demand for billing accuracy and compliance systems |
|
Fraud & Program Integrity |
Centers for Medicare & Medicaid Services – Program Integrity Initiatives |
Focus on detecting fraud, waste, and abuse; billions recovered annually |
Drives adoption of AI-based fraud detection and risk mitigation tools |
|
Reimbursement Scale |
Centers for Medicare & Medicaid Services – Medicare Program |
Covers 65M+ beneficiaries, making it the largest payer with strict claim validation processes |
Creates large-scale opportunity for revenue optimization solutions |
Uncover macros and micros vetted on 75+ parameters: Get instant access to report
How is the expansion of autonomous RCM platforms creating new growth opportunities in the U.S. healthcare revenue integrity market?
The increasing number of claim denials and incidents of misconduct in the U.S. healthcare system offer immense opportunities for AI-driven revenue integrity services, particularly services aimed at preventing claim denials and optimizing documentation. The CMS indicates that the Medicare Fee-for-Service program sees an improper payment rate hovering around 6.55%. This equates to a substantial USD 28.83 billion in 2025. A significant portion of this amount can be traced back to insufficient documentation and operational inefficiencies. (Source: Centers for Medicare & Medicaid Services (CMS)
Moreover, as per statistics from KFF on federal marketplaces, approximately 19% in-network claims and 37% of out-of-network claims were rejected in the U.S. during 2023. This highlights a great potential lies in the application of artificial intelligence technology for the purposes of code and documentation validation, as well as predictions about claim denials. (Source: Kaiser Family Foundation)
Market Players, Key Development, and Competitive Intelligence

To learn more about this report, Request Free Sample
Key Developments
- In May 2025, New Mountain Capital announced its integration of SmarterDx, Thoughtful.ai, and Access Healthcare with an objective of developing a technology-driven platform for clinical documentation, coding accuracy, and revenue cycle optimization. This is an indication of the growing role of AI technology in enhancing revenue integrity with fewer coding errors.
- In May 2025, Optum, Inc. launched an artificial intelligence-powered revenue cycle management solution with an aim to improve accuracy in claims, reduce denials, and increase efficiency in reimbursement. This shows that there is a move towards using artificial intelligence-powered automation in revenue integrity to ensure that there is no loss of revenue.
- In March 2024, the UnitedHealth Group update on the Change Healthcare cyber-attack indicated a considerable disruption in claims processing, billing, and payment processes in the U.S. healthcare system. This attack highlights the importance of robust and secure revenue cycles and revenue integrity solutions, thereby fueling investment in cybersecurity, data security, and artificial intelligence-based security measures in RCM solutions.
Competitive Landscape
The market for healthcare revenue integrity in the U.S. is very competitive and changes quickly. Big healthcare IT companies, specialized RCM service providers, and AI-driven startups are helping providers to enhance financial outcomes. Market players are increasingly focusing on automating, integrating AI, and improving the whole revenue cycle to reduce the number of claims that are denied, making sure that coding is correct, and that they follow the rules. Key focus areas include:
- AI-Driven Coding Accuracy and Denial Prevention Solutions
- End-to-End Revenue Cycle Management (RCM) Platform Integration
- Regulatory Compliance and Audit Optimization Capabilities
Market Report Scope
U.S. Healthcare Revenue Integrity Market Report Coverage
| Report Coverage | Details | ||
|---|---|---|---|
| Base Year: | 2025 | Market Size in 2026: | USD 3,448.8 Mn |
| Historical Data for: | 2020 To 2024 | Forecast Period: | 2026 To 2033 |
| Forecast Period 2026 to 2033 CAGR: | 8.6% | 2033 Value Projection: | USD 5,692.5 Mn |
| Segments covered: |
|
||
| Companies covered: |
Optum, Inc., Epic Systems Corporation, Oracle Cerner, R1 RCM Inc., McKesson Corporation, Conifer Health Solutions, Experian Health, athenahealth, Inc., Veradigm, and Medical Information Technology, Inc. |
||
| Growth Drivers: |
|
||
| Restraints & Challenges: |
|
||
Uncover macros and micros vetted on 75+ parameters: Get instant access to report
Analyst Opinion (Expert Opinion)
- The U.S. healthcare revenue integrity market is on the cusp of a major transformation, driven largely by artificial intelligence, automation, and predictive technologies. Advanced analytics are set to become a key player, enabling the identification of revenue leakage, coding mistakes, and potential claim denials before a single claim is filed. The market is moving from a reactive approach to revenue cycle management. Instead, the focus is on real-time, intelligence-driven financial optimization. This transformation is being fuelled by cloud-based platforms and better integration with clinical systems.
- The most promising prospects reside in artificial intelligence-driven coding and denial prevention systems tailored for expansive hospital networks within the U.S. Substantial inefficiencies are inherent in the current landscape, stemming from elevated claim volumes and intricate reimbursement protocols. With payers imposing more rigorous standards and the proliferation of value-based care models, healthcare providers are progressively channelling resources into automated revenue integrity solutions, thereby ensuring adherence to regulations and maximizing reimbursement results.
Market Segmentation
- Type Insights (Revenue, USD Mn, 2021 - 2033)
- Billing and Invoicing
- Medical Coding Services
- Claims Management
- Denial Management
- Revenue Cycle Assessment and Analysis
- Charge Capture Audit Services
- Managed Care/Payer Contract Management
- Others
- Component Insights (Revenue, USD Mn, 2021 - 2033)
- Services
- Platforms
- Deployment Model Insights (Revenue, USD Mn, 2021 - 2033)
- On-Premises
- Cloud-Based
- Others
- End User Insights (Revenue, USD Mn, 2021 - 2033)
- Hospitals and Clinics
- Individual Practitioners
- Ambulatory Surgical Centers
- Others
- Key Players Insights
- Optum, Inc.
- Epic Systems Corporation
- Oracle Cerner
- R1 RCM Inc.
- McKesson Corporation
- Conifer Health Solutions
- Experian Health
- athenahealth, Inc.
- Veradigm LLC
- Medical Information Technology, Inc.
Sources
Primary Research Interviews
- Revenue Cycle Director – Multi-hospital health system (U.S.)
- VP, Revenue Integrity – Large academic medical center
- Head of Coding & Clinical Documentation Improvement (CDI)
- Director – Denial Management & Claims Audit
- CFO / Finance Head – Hospital network (billing & reimbursement focus)
Databases
- Centers for Medicare & Medicaid Services – Claims, reimbursement, improper payment data
- American Hospital Association – Hospital financial performance & billing trends
- Healthcare Financial Management Association – Revenue cycle benchmarks
- Medical Group Management Association – Physician billing & denial trends
- Kaiser Family Foundation – Healthcare spending & payer mix
Magazines
- HFMA Magazine (Healthcare Financial Management Association)
- Journal of AHIMA (American Health Information Management Association)
- Becker’s Hospital Review
- Modern Healthcare
- Healthcare Business Monthly (AAPC)
- Revenue Cycle Advisor (DecisionHealth)
- HIMSS Media / Healthcare IT News
Journals
- Journal of AHIMA (coding, CDI, compliance)
- HFMA Publications (Revenue Integrity & Financial Performance)
- Journal of Healthcare Finance
- Becker’s Hospital Review (RCM trends & company activity)
Newspapers
- The Wall Street Journal
- Financial Times
- The New York Times
- USA Today
- The Washington Post
- Los Angeles Times
- Chicago Tribune
Associations
- Healthcare Financial Management Association
- American Health Information Management Association
- Centers for Medicare & Medicaid Services
- U.S. Department of Health and Human Services
Public Domain Sources
- Centers for Medicare & Medicaid Services (CMS)
- U.S. Department of Health and Human Services (HHS)
- Centers for Disease Control and Prevention (CDC)
- Office of Inspector General (OIG)
- Medicare Payment Advisory Commission (MedPAC)
- Agency for Healthcare Research and Quality (AHRQ)
- National Institutes of Health (NIH)
- Bureau of Labor Statistics (BLS)
- U.S. Census Bureau
- Government Accountability Office (GAO)
Proprietary Elements
- CMI Data Analytics Tool, Proprietary CMI Existing Repository of information for last 10 years.
Share
Share
About Author
Komal Dighe is a Management Consultant with over 8 years of experience in market research and consulting. She excels in managing and delivering high-quality insights and solutions in Health-tech Consulting reports. Her expertise encompasses conducting both primary and secondary research, effectively addressing client requirements, and excelling in market estimation and forecast. Her comprehensive approach ensures that clients receive thorough and accurate analyses, enabling them to make informed decisions and capitalize on market opportunities.
Missing comfort of reading report in your local language? Find your preferred language :
Transform your Strategy with Exclusive Trending Reports :
Frequently Asked Questions
EXISTING CLIENTELE
Joining thousands of companies around the world committed to making the Excellent Business Solutions.
View All Our Clients